 A patient with a history of possible SVT may have first degree AV block because of the presence of “dual AV node physiology,” which is the presence of two pathways to the AV node that predispose to AV node reentry SVT, the most common type of SVT with onset in the adolescent and teen years. These individuals will have a murmur and may also have IVCD (see above). With an atrial septal defect, the atrial enlargement can prolong the time for conduction from the sinus node to the AV node. Pathological causes for this relate to the underlying reason for the first-degree AV block. The majority of cases are normal variants. 
This refers to PR prolongation >200msec however, it is a rate-dependent definition, thus shorter intervals at low heart rates also qualify. Cardiology evaluation is recommended for >120 degrees. Most of these are normal in the range of 90-100 degrees. If the mean QRS vector is greater than -10 degrees (example -30 degrees), cardiology evaluation is warranted as is the case if there is LAD along with other findings (T wave inversion, atrial enlargement, conduction delay, etc.) Right Axis Deviation (RAD) In infants or children with murmurs or a family history of cardiomyopathy, cardiology evaluation is warranted. However, the reason for performing the ECG in part should dictate whether cardiology evaluation is warranted. It is frequently a normal variant in asymptomatic older children. Other causes include left-sided heart disease, single ventricles, and cardiomyopathies. Cause for concern is that it can be associated with an AV canal defect or inlet VSD. This refers to the mean QRS vector being less than 0 degrees. Holter monitors interpreted by non-pediatric cardiologists may label this as recurrent SVT. Frequently these situations result in sinus tachycardia because of the fear reaction. Unfortunately, when it is very pronounced, it can be a cause for concern in the patient or parents who interpret the irregular rhythm as abnormal or possibly (in medical families) as a sign of atrial fibrillation. This is invariably normal and physiologic. If a murmur is present or there are potential cardiac symptoms or the QRS duration is >120msec cardiology evaluation is warranted. Sometimes medications can cause conduction delay, this is felt to be benign. But since there is a small proportion of patients who do have an abnormality, a decision on whether or not the patient should be evaluated further depends on the reasons for the electrocardiogram.Ĭause for concern: This may be a manifestation of RV enlargement in situations such as an atrial septal defect or anomalous pulmonary venous return.  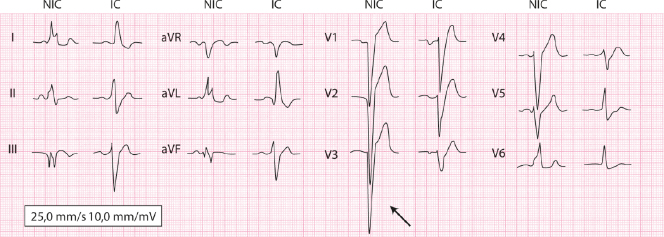
The difficulty for cardiologists reading an electrocardiogram with conduction delay without seeing the patient is that it is tempting to label it as normal since the vast majority of the patients with this, in fact, have a normal heart. It is mostly a variant of normal, especially in athletes. This is also known as conduction delay, IVCD, or incomplete right bundle branch block (iRBBB). This is a brief review of the terminology and implications of ECG interpretations to assist providers in their decision making. The physician receiving ECG results may question what these mean in some instances, what is significant and finally, what to do with the results. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
